As there are no right or wrong questions when it comes to eye loss, if you cannot see the answer here please do not hesitate to email us.
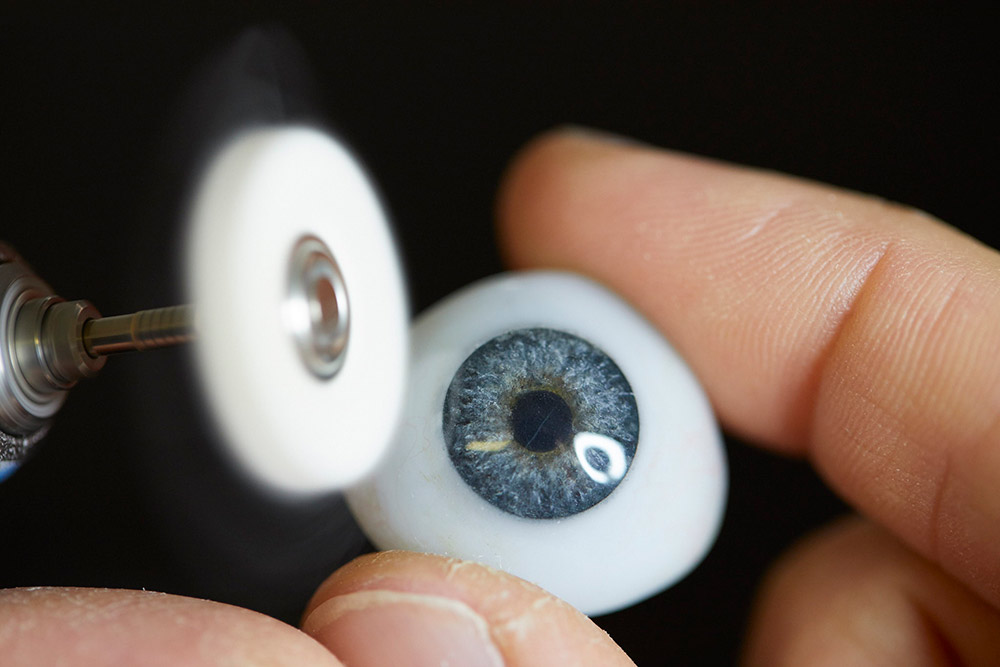
What is a bespoke ocular prosthetic?
A bespoke craftsman such as a tailor makes things that are specially made for the customer.
We take pride in using this technique and believe in it completely. Our eyes are 100% custom made with all parts made in house using the highest quality materials, we do not employ any outside or third parties for this.
Taking an impression and using the lost wax technique, we get the best possible fit resulting in the best possible outcome. The benefits from using the Bespoke technique are improved comfort, precise gaze and greater motility of the eye.
Does it hurt to wear an ocular prosthetic?
A well-made prosthesis should feel comfortable to wear without any pain. In some cases, you may need to build up a tolerance to wearing a prosthesis. At the wax stage of the build you will be able to tell if anything isn’t feeling quite right, if you have a good Ocularist you can work together at this point to make it the most comfortable fit possible.
Will my ocular prosthetic fall out?
Our goal as your Ocularist is to get the best fit possible, which means the prosthesis should sit within the socket without any risk of it falling out. In some cases where there is Lower Lid Laxity upon consultation we would refer you on to an Oculoplastic surgeon to discuss your options.
How often does a prosthetic eye need to be replaced?
Prosthesis replacement is dependent on the age of the patient. In adults, we suggest every 3-4 years. This is because as we age our socket shape changes as does our iris and sclera colour.
In children, this can vary greatly dependant on age. As an example, a new born through to the age of two can require up to 15 prosthesis including conformers. However, this will slow up drastically after the age of two years when the rate of growth slows.
Why should I get it polished every four to six months?
As the prosthesis is made of acrylic your bodies proteins can eat into the top layer of PMMA. This is on a micro scale but is enough to slow the motility and dull down the natural glisten of the prosthesis reducing realism. Polishing also helps to maintain the hygiene and health of the socket. This is also a good opportunity to have a check-up and see how things are going. Artificial Eye Care is something that you can ask your Ocularist about also.
Can I swim with my prosthesis in?
You can swim with it in, however you would need to be a little bit more careful than someone without a prosthesis. Some people feel more comfortable with the prosthesis out as they would rather not run the risk of losing it.
Can I get a designer eye?
Please do….. Oculus Prosthetics is one of the only clinics in the world offering this service and we love it.
What does an Artificial Eye Cost?
Artificial Eye Cost varies from country to country quite considerably. We charge $2400 for a fully bespoke prosthesis which includes your first consultation and review.
Terminology
Definitive Prosthesis: Bespoke Moulded, hand painted artificial eye.
Cosmetic Shell: Thin full surface shell hand made in PMMA to cover disfigured or phthisical eye.
Conformer: Plastic shield placed within the fornices of the socket at the final stages of enucleation/evisceration to maintain the forniceal depth and to help reduce post-op swelling.
Socket Expander: Can be hydrophilic, absorbs liquid therefor stretches small underdeveloped sockets/soft tissue.
Enucleation: Surgical removal of the whole eye (globe) and dissection of the globe from the optic nerve.
Evisceration: Surgical removal of the contents of the eye without optic nerve or muscle disturbance.
Exenteration: Surgical removal of the eye, the orbital contents, eye lids and surrounding tissue.
Microphthalmos: The under development of the human eye, often picked up in baby scans. More commonly known as Microphthalmia.
Anophthalmos: Non-development of the human eye or eyes. Post enucleation the patient is rendered Anophthalmic.
Glaucoma: Raised intra-ocular pressure, treated with eye drops, can be painful and end up in endophthalmitis.
Macular Degeneration: The macular hole becomes diseased, two types wet and dry. Treatment currently not very successful however this is attracting a lot of research.
Retinal detachment: Where part or all of the retina becomes torn or dislodged. Treatment can be laser or glue to re-attach the retinal tissue.
Book your free online consultation
Contact Oculus Prosthetics today to schedule your complimentary 30-minute chat with ocularist Dwayne Collins.



